Review Article
Year: 2021 |Volume: 2 | Issue: 04 |Pages: 20-32
SYSTEMIC REVIEW OF GANDUSH DRUGS AGAINST ORAL CARE W.S.R. TO ASHTANG HRUDAYA
About Author
Correspondence Address:
Dr.Sandeep Kisan Rajput- Associate Professor Balrog Department YMT Ayurved College and Hospital, Kharghar E-mail – dr.rajputsandeep@gmail.com
Date of Acceptance: 2021-04-28
Date of Publication:2021-05-01
Article-ID:IJIM_69_05_21 http://ijim.co.in
Source of Support: NIL
Conflict of Interest: NIL
How To Cite This Article: Rajput SK. , Pawar U, Irole SA., & et.al. Systemic Review Of Gandush Drugs Against Oral Care W.S.R. To Ashtang Hrudaya.Int. J Ind. Med. 2021;2(4):20-32
Abstract
The name of Ayurveda originates from two Indian words Ayu means life and Veda means knowledge. In a broad sense it means knowledge concerning the maintenances of life. Ayurveda is an ancient science of life from 5000 years. There are no if and or buts about it oral health is a huge part of our general health and a welled balanced. Oral diseases continue to be major health problem world wild there for it is very important to maintain oral hygiene for maintenance of health and longevity of human Being in particular age group . Older age groups are also at increased risk mouth dryness for example due to lack of saliva etc. In ancient Ayurvedic text have medicinal and cariogenic property. Its oil pulling practice in various systemic diseases. If traditional medicine is to be acknowledge as part of primary health Care scientific validation of the Ayurvedic dental health practices could justify their incorporation into modern dental Care. Ayurveda recommends Gandusha as a specialized therapy for good oral hygiene. It will maintain and promote the oral hygiene by exerting the cleansing action and by increasing the defense mechanism in the oral cavity. Gandusha is used for both prevention and treatment of oral diseases. The present review article highlights how the Gandusha therapy will act as a basic tool for good oral hygiene.
Keywords: Gandush, oral health, mouth. Stomatitis
Introduction
Mouth is considered as the mirror of the health of human body. (1) Oral cavity harbors billions of microorganisms ; some of these contribute to the development or progression of systemic diseases such as cardiovascular disease, diabetes mellitus etc. oral health and general health are interrelated.(2) Oral disease continue to be a major health problem world wide .So it is important to maintain the oral hygiene for maintenance of the general health in society. (3) The main aim of Ayurveda is to preserve the healthy person remains as healthy and also treat or cure the person who is suffered from any diseases in such way that the disease is snatch away from its root cause.(4) Gandush upkram is recommends as a dincharya upkram for prevention and promotion of good Oral health.(5) Oral cavity is such a part of the body which is constantly exposed to many risk factors in day to day life. And risk of oral disorders is also increased so it is very important to maintain oral health. Regular practice of Gand?sha will help to regain good oral hygiene. In Ayurveda, Gand?sha is explained as one of the routine procedures under the context of daily regimens (dinacharya)6 3,4 It can be done in both healthy and disease person.
Gandush you fill the liquid or oil in the mouth fully so there is no movement in your mouth and so your mouth is completely distend, and it is held until there is lacrimation, nasal discharge and then patient is spit this out. This process is very good for teeth and it vanishes all the impurities and toxins, it stretches your check muscles therefore several reasons why you do that.(7) Types of gandush as follows: (8,) 1.Snidgha gandush 2.Shaman gandush 3. Shodhan gandush 4.Roopan gandush. Indication of gandush: (9) 1. Tingling of teeth 2.disease of mouth caused by vata 3.shaky teeth Indication of gandush : (10) 1. Dryness of mouth 2.cracking lips 3.sensitivity 4.dental pain. In this article, we are tried to review the various Gandush drugs and its benefits as well as action on oral disease of oral cavity. So there are many formulations for gandush are available in Ayurvedic text, we are focusing on only 2 formulations which are explained in Ashtang Hridaya.
Aims- To evaluate Doshagana Properties in formulation of Gandush & Kaval.
Objective – To find out the drug efficacy with the help of their properties like Rasa Virya Vipak
Material and Methods :
Procedure : The person shoulder face & neck should be massaged & fomented. Keeping his face slightly lifted up. He should hold the liquid in his mouth till the mouth get filled with kapha till the nose and eyes become secretory after which it is spat out.(11)
Schedule for Gandush : The medicated fluid or medicated paste is kept in mouth with concentrated mind without any swiss movement till the collection of kapha in mouth , nasasrava (running nose) , and netrasrava ( watering of eyes ) then the fluid is spit out (12)
Indication for Gandush : Dantaharsh ( tingling of teeth ), DantaChala ( shaky teeth ), Mukha roga Vataj ( disease of mouth cause by vata ). Gandush of water mixed with paste of tila in lukewarm state of cold.(13)
Benefits of kaval : Swarabhed ( strength of voice ), hanubalam ( strength of jaws ), strength of face, better taste perception , strong & healthy teeth, Resistance again Doshaja or Agantuja Mukharog , (14) . Regular practice of gandush till tail with not suffering from Kantashosha ( dryness of mouth ) , Oshtasputana ( cracking lips ) , Dantakshaya ( loss of teeth ) Dantashula ( dental pain ) Dantaharsha ( sensitivity ). (15)
Samyak lakshana of kaval : vyadhiapachaya ( disease subside ) Trushti ( feeling of freshness ) Vaishadya ( cleansing effect ) Vaktralaghuta ( lightness of mouth ) , Indriyaprasada ( clarity of sense Organ ) (16)
Hinayoga lakshana of kaval : stiffness, excitation of kapha , loss of test (17)
Atiyog lakshana of kaval : mukhapak ( stomatitis ), sosa ( dryness of mouth ) , Trushna ( thirst ) arucchi ( anorexia ) , klama ( exhaustion ) (18)
Formation 1: Ashtang hridaya; Uttar tantra, 22/104. The ingredients of 1st formulation: Patol, Shunthi, Triphala, Indrayan, Trayman, Kutki, Haldi, Daruharidra, Guduchi, Madh (19)
Formulation 2: Ashtang hridaya; Uttar tantra, 22/107. The ingredients of 2nd formulation: Khadir, Agaru, Triphala, Arjun, Madyanti, Irimed. (20)
Observation -
FORMULATION: 1
1. PATOLA: Pharmacological activity : Patol have chemo preventive activity, Antihyperglycemic and Antihyperlipedemic activity, laxative activity, anti-inflammatory and anti-nociceptive activity, cholesterol lowering activity.(21)
2. Shunthi: Shunthi stimulates digestion, absorption, relieve constipation and flatulence by increasing muscular activity in the digestive tract (22) as well as it significantly reduces nausea and vomiting. (23) it is good suppressant of gut colic and diarrhoea. (24) Shunthi could be used as a anti-thrombotic and anti-inflammatory agent.(25)
3. TRIPHALA:
a) AMLA: Pharmacological activity on amla: Antioxidant (26) hypoglycemic, anti-inflammatory, Antihyperglycemic, Antihyperlipedemic,(27,) antipyretic, analgesic, antitussive, antiatherogenic, adaptogenic, cardioprotective, gastroprotective, antianemic, wound healing, anti-atherosclerotic, hepatoprotective,. In addition, experimental studies have shown that amla and some of its phytochemicals such as Gallic acid, ellagic acid, pyrogallol, some norsesquiterpenoids, corilagin, geraniin, elaeocarpusin, and prodelphinidins B1 and B2 also possess antineoplastic effects. Amla is also reported to possess radio modulatory, Antimutagenic effects decreases lipid peroxidation decreases ornithine decarboxylase radio protective agent chemo preventive agent (28).
b) BIBHITAK: Pharmacological effects as follows: Analgesic activity , Antihypertensive effect (29), Antispasmodic and Bronchodilator properties (30), Antimicrobial activity (31) Antioxidant activity (32), wound healing activity (33), immunological activity (34), Acute – subacute toxicities (35) Hepatoprotective activity (36),
c) HARITAKI: Haritaki is used to treat Ophthalmic, itching, edema (37) it is used as an Antioxidant and neuroprotective drug (38). This plant is also used for treating piles, dropsy, diarrhoea, biliousness, headaches, dyspepsia and ascites [39].It is also used for heart disease, inflammation, brain dysfunction [40] .
4. INDRAYAN: Pharmacological activities 0f Indrayan: Indrayan have antioxidant activity (41), Anti hyperlipidemia activity (42), Anti fertility by decrease level of cholesterol (43), anti-microbial of alkaloids’ (44), anti-diabetic effects by glycosides (45)
5. TRAYMAN: The roots of the plant are used as bitter tonic, antiperiodic, expectorant, astringent, stomachic, anthelmintic, antipsychotic, anti-inflammatory, sedative antibacterial. (46)
6. KUTAKI: Kutaki is used as medicine for cough, cold; fever (47).It is used to cure jaundice, diarrhoea and dysentery. (48) Pharmacological activity: Kutki have Antimicrobial activity (49), antibacterial activity (50), cytotoxicity (51), anti-mutagenic activity (52), nephroprotective activity (90), anti-inflammatory activity (53), and antioxidant activity (54).
7. HALDI: Turmeric enhances wound healing (55).Turmeric lower serum cholesterol levels (56).Extract of turmeric suppresses symptoms associated with arthritis (57) Turmeric protects against pancreatitis (58). Turmeric extract corrects cystic fibrosis defects (59) Turmeric constituents inhibit scarring (60)
8. DARUHARIDRA: Berberis aristata DC . Commonly knowns as Daruharidra are a popular drug which has been used globally. Charak Samhita prescribed that the extract of the plant be taken internally for treatment of hemorrhage, piles, pruritus, shotha (Inflammation), eye disease and alopecia. Described it as being useful internally in indigestion, deficiency of breast milk, and in uterine and vaginal disorders. (61) Treat allergies, metabolic disorders, ophthalmic, and other eye diseases, treat bleeding piles, anti-osteoporosis, treat skin diseases, menorrhagia, fever, diarrhea, dysentery cholera, jaundice, ear infections, anti-bacterial, anti-fungal, anti-inflammatory analgesic, anti-pyretic, anti-diabetic, and anti-hepatopathic (62)
9. GUDUCHI: Guduchi mentioned in Ayurvedic text of Ayurvedic system of medicine like Charak, Sushrut, Ashtang Hridaya and other varies text like Bhavprakash, Dhanvantari Nighantu. (63) Tiktaa- saka varga (vegetables) and claimed to be useful in treating fever, asthma, anorexia. (64) Indicated in fever, gout, jaundice. (65) Skin infections, chronic diarrhoea, and dysentery like G.I.T infection. (66) To cure bleeding piles, curing itching, erysipelas. (67)Guduchi mainly contains alkaloids, glycosides, steroids, sesquiterpenoids, aliphatic compounds, essential oils, mixture of fatty acids and polysaccharides. The alkaloids include berberine, bitter gilonin, non-glycoside gilonin gilosterol. (68)
10.MADH: Pharmacological Effects: Madh have antioxidant activity (69), Antimicrobial activity (70), Antifungal effect, Antiviral activity (71), Anti-inflammatory activity (72).
FORMULATION 4TH :
- KHADIR:
Khadir is used as medicine for Asthma, cough, diarrhea, and dysentery, boils, in skin infection and sores and for stomatitis. The plant part used as astringent, bactericide, refrigerant, stimulant .The bark is used as a antipyretic, anti-inflammatory, in bronchitis, ulcers, anemia. (85) used for expel worms, heal wounds, and suppress the coughing (86)
- AGARU :
Agaru reduces cough and helps in Bronchitis and asthma. Agaru is used as s mouth freshener. Because of its cooling effect it is used in fever associated with chills both internally and externally. It may be used in toothache, headache. Pharmacological effect of Agaru having Antioxidant, Hepatoprotective activity , Anti-inflammatory activity, Anti diabetic activity, Anti-pyretic activity, Analgesic activity, Anti histamine activity, Laxative effect, Anti-microbial activity (87) .
- TRIPHALA: As mentioned in formulation 1.
- ARJUN:
Bark of Arjuna is used in the fever and high blood pressure. Bark and juice of arjuna is used as Antacid (88) It is also used in treatment of snake bite and scorpion sting(89)
- MADYANTI :Pharmacological activity having Analgesic and antipyretic activity , Anti-inflammatory activity, Anti-arthritic activity (90), Anti-ulcer activity , Anti diabetic activity Anti-fungal activity(91) Antiviral activity ,Antimalarial activity Anti fertility activity (92)
- IRIMED :Pharmacological activity: Irimed having anti-inflammatory activity, Anti-cancer activity, anti-obesity, antiaging activity. Hepatoprotective activity, anti-diabetic properties (93), Antimicrobial activity , anthelminthic , antioxidant (94) .
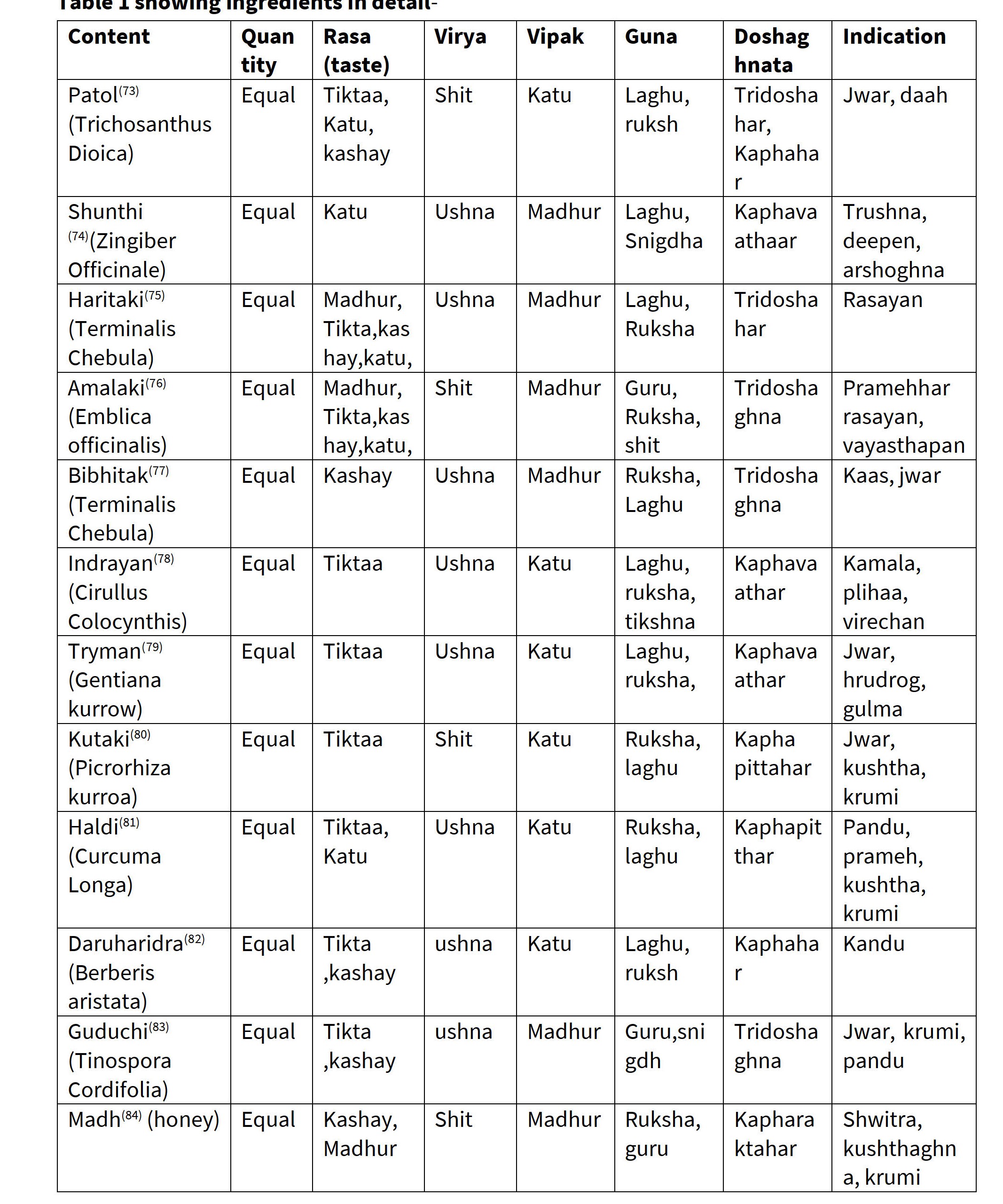
table 1
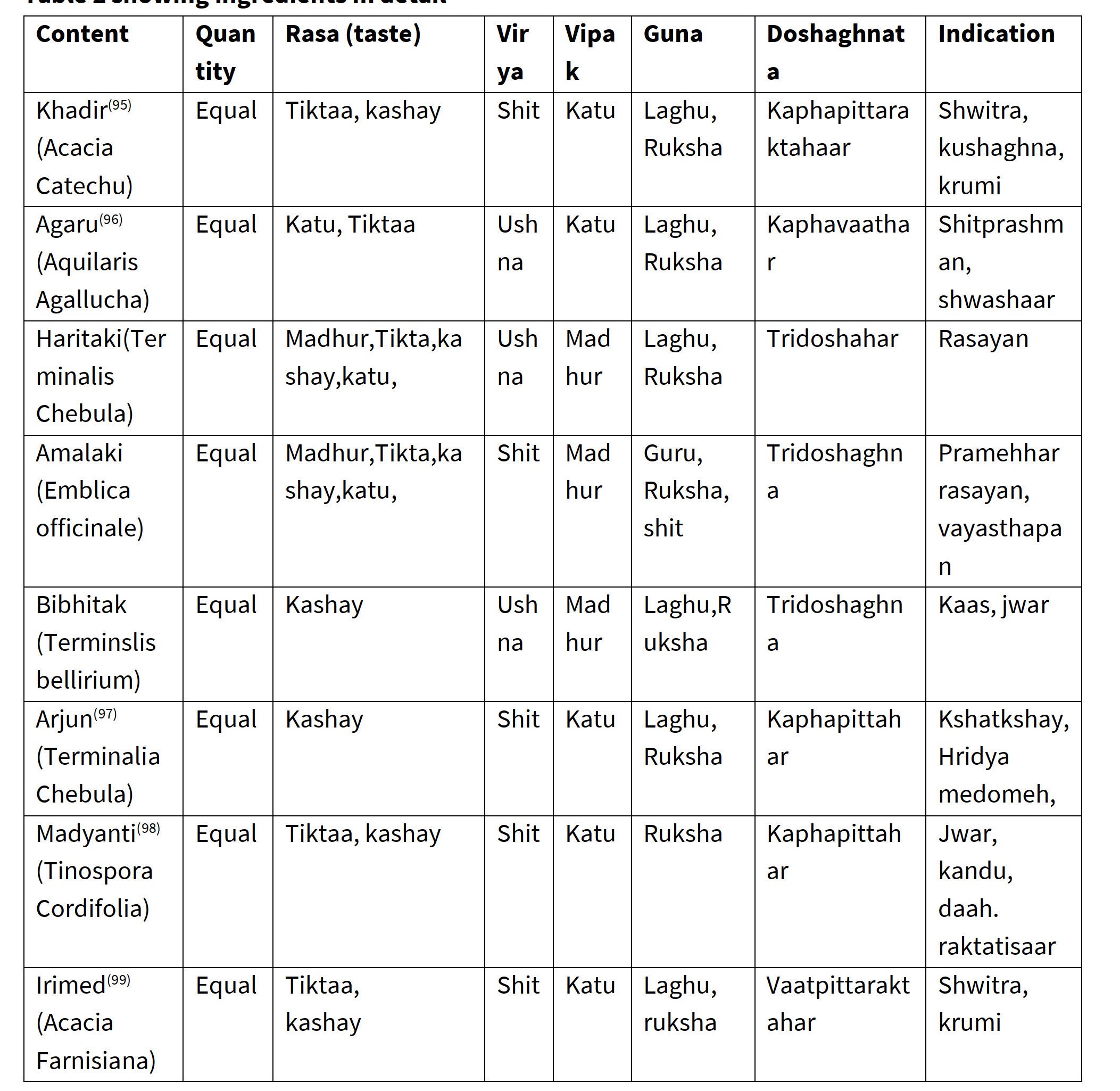
table 2
Discussion
Mode of action Gandoosha and Kavala
The saliva consists of lysozyme, an enzyme and antibody IgA, which are bacteriostatic and antimicrobial in nature. The Gandush and Kavala increase the pressure in the mouth, which stimulates the stretch reflex i.e. the presso receptors resulting in stimulation of the salivary nuclei in brain stem. This results in increased activity of parasympathetic motor fibers of facial and glossopharyngeal nerves and increases the salivary output, which is further stimulated by the chemical constituents stimulating the oral chemo receptors and hence the Gandush and Kavala maintains and cures the oral environment.[100]
Formulation 1: In this formulation the drugs are Chemo protective, hyperlipidemia, anti-inflammatory, Anti-thrombotic, they act on GIT. They have ushna Virya, Tiktaa Katu, kashay ras, and Katu Vipak so mostly acts on vata vikar.
Formulation 2: the dugs are act on stomatitis, ulcers, G.I.T., URTI and worms and Urdhwajatrugat Vikar. They have anushnashit , Laghu, Ruksha properties so they are Tridoshaghna according to Ayurveda.
Conclusion
Above formulations are based on dosh samprapti. So according to Doshaghnata we can use the drugs. This is our small efforts how these drugs will be act by their Doshaghnata as well by their qualities. Gandush upholding the internal hygiene of body as well as cure the disease specifically related head, neck, ears, mouth & eyes. Oral route is common way for entry of various micro-organisms that which are going to cause illness to oral area & systemic illness. Gandush bioactive ingredients present in the drug having property Anti-inflammatory, Immuno- modulatory & Anti-oxidants. Gandush to prevent the entry of causative micro-organisum.
References
1. Vagish Kumar, Review article oil pulling for maintaining oral hygiene journal of traditional & complementary medicine 2017 7: 106e109. journal homepage: http://www.elsevier.com/locate/jtcme.
2. Vagish Kumar, Review article oil pulling for maintaining oral hygiene journal of traditional & complementary medicine 2017 7: 106e109. journal homepage: http://www.elsevier.com/locate/jtcme.
3. Nilesh A,T., Sudhir H., Pankaj G Role of Ayurveda in management oral health PMCID:PMC3931197 , https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3931197/ .
4. Prevention and treatment of diseases of mouth by gandoosh and kavalusujatasooryavanshi and b. r. mardikarbharatividyapeeth’s college of ayurveda, erandwane, pune – 411 038, india
5.Agnivesha. Charaka Samhita, Comm. Chakrapanidatta. In: Jadavaji TA, editor. Sutrasasthana. Varanasi: Chaukhamba Surbharati Prakashana, 2008. 5/78-81: 27
6. Triphala, a New Herbal Mouthwash for the Treatment of Gingivitis: A Randomized Controlled Clinical Trial.;Pradeep AR, Suke DK, Martande SS, Singh SP, Nagpal K, Naik SB.; J Periodontol. 2016 Nov; 87(11):1352-1359. Epub 2016 Jul 21.; PMID: 27442086
7. Ambika datta. SushrutaSamhita, Vol-1, CHIKISTA STHAN 40/62, Chaukhambha
8.K.R. Srikantha Murthy, Astanga Hrdayam, sutra sthana, Chowkhamba Krishnadas Academy, Varanasi. 1(22): 1,269:
9.Priya Vrat Sharma, Susruta Samhita, volume-2,Chikitsa sthana, chapter 40,verse no:60-61, page no 681 Chaukhambha Visvabharati,Varanasi.
10.K.R.SrikanthaMurthy,Astanga Hrdayam,vol-1,sutra sthana , chapter 22,verse no-12,page no-271,Chowkhamba KrishnadasAcademy,Varanasi.
11. P.V. Sharma, Susruta Samhita, vol-2, Chikitsa sthana, chapter 40,verse no:56, Chaukhambha Visvabharati, Varanasi.
12. K.R. Srikantha Murthy, Astanga Hrdayam,vol-1,sutra sthana , chapter 5 ,verse no-79,page no-72 , Chowkhamba Krishnadas Academy, Varanasi.
13. Priya Vrat Sharma, Susruta Samhita, volume-2,Chikitsa sthana, chapter 40,verse no:60-61, page no 681 Chaukhambha Visvabharati,Varanasi.
14. critical analysis of role of kaval and gandush in the management of halitosis krithi amai1 www.jahm.in (ISSN-2321-1563)
15. K.R. Srikantha Murthy, Astanga Hrdayam,vol-1,sutra sthana , chapter 22 ,verse no-12 , page no-271 , Chowkhamba Krishnadas Academy, Varanasi.
16. International Journal of ayurvedic medicine http://iijam.co.in ISSN:0976-5921 , 2014,5(2),148-153.
17. Priya VratSharma, Susruta Samhita, volume 2 Chikitsa sthana, (40): 63. Chaukhambha Visvabharati, Varanasi.
18. Priya VratSharma, Susruta Samhita, volume 2 Chikitsa sthana, (40): 64. Chaukhambha Visvabharati, Varanasi.
19. Pt. Shastri Kashinath,Ashtang Hridaya,Krishnadas Academy Varanasi chaukumba press, edition 1994, 22/104 Pp-523.
20. Pt. Shastri Kashinath,Ashtang Hridaya,Krishnadas Academy Varanasi chaukumba press, edition 1994, 22/107 Pp-523.
21. Gupta vikas,Pagoch S S,Pharmacological review of Trichosanthes Dioica (patola), International journal, ISSN:2320 5091, Volume 2, Issue 3, May –June 2014
22. Stewart J, Wood MJ, Wood CD and Mims ME, Effects of ginger on motion sickness susceptibility and gastric function. Pharmacology, 1991; 42: 111.
23. Ernst E and Pittler MH, Efficacy of gingerfor nausea and vomiting. A systematic review of randomised clinical trials. Br J Anaesth, 2000; 84: 367.
24.Ghayur MN, Gilani AH, Ginger lowers blood pressure through blockade of voltage dependent calcium channels. J.Cardiovasc. Pharmacol, 2005; 45: 74–80.
25. Thomson M, Al-Qattan KK, Al-Sawan SM, Alnaqeeb MA, Khan I, Ali M, The use of Ginger (Zingiber officinale Rosc.) as a potential anti-inflammatory and antithrombotic agent.
26. V.D. Reddy, P. Padmavathi, G. Kavitha, S., Emblica officinalis ameliorates alcohol-induced brain mitochondrial dysfunction in rats,J. Med. Food 14 (1–2) (2011) 62–68
27. B.Antony, M. Benny I.N.B.Kamal A Pilot Clinical study to evaluate the effect of Emblica officinalis extract (Amlamax™) on markers of systemic inflammation and dyslipidemia, Indian J. Clin. Biochem. 23 (4) (2008) 378–381.
28. Lippincott Williams & Wilkins. Unauthorized reproduction of this article is prohibited. European Journal of Cancer Prevention 2011, Vol 20 No 3 , Page No. 215-230
29. Arif-Ullah Khan, Anwarl Hassan Gilani. Pharmacodynamic Evaluation of Terminalia belerica for its Anti-Hypertensive Effect. Journal of Food and Drug Analysis. 2008; 16:6-14
30. Anwarul Hassan Gilani, Arif-Ullah Khan, Tuba ali. Anti-Spasmodic and Bronchodilatory Properties of Terminalia belerica Fruit, Journal of Ethnopharmacology. 2008; 116:528-538.
31. Elizabeth KM. Anti-microbial Activity of Terminalia belerica. Indian Journal of Clinical Biochemistry. 2005; 20(2):150-153.
32. Ramesh Kumar, Chauhan PK, Munish kumar. In vitro investigations of antioxidant and phytochemical activities of aqueous extracts of Terminalia belerica & Terminalia chebula International Journal of Research in Pharmaceutical and Biomedical Sciences.
33. Saha PK, Patrab PH, Pradhan R. Effect of Terminalia belerica & Terminalia chebula on wound healing in induced dermal wounds in Rabbits. Pharmacology online 2011; 2:235-241.
34. Aurasorn Saraphanchotiwitthaya, Pattana Sripalakit and Kornkanok Ingkaninan. Effects of Terminalia belerica Roxb. Methanolic extract on mouse immune response in vitro, Maejo International Journal of Science and Technology. 2008; 02(2):400-407.
35. Thanabhorn S, Jaijoy K, Thamaree S, Ingkaninam K. Acute and Sub-acute Toxicities of the Ethanol Extract of fruit of Terminalia belerica Journal of Pharmacuetical sciences, 2009.
36. Pinmai K,. Synergistic growth inhibitory effects of Phyllanthus emblica and Terminalia bellerica extracts with conventional cytotoxic agents: Doxorubicin and cisplatin against human hepatocellular carcinoma and lung cancer cells. World J Gastroenterol. 2008; 14(10):1491-97.
37. Chia Lin Chang and Che San Lin, Phytochemical Composition, Antioxidant Activity and Neuroprotective Effect of Terminalia chebula Retzius Extracts, EvidenceBased Complementary and Alternative Medicine , Volume 2012, Article ID 125247, 7 pages
38. Pulliah T, Encycllopedia of world Medicinal Plants, Volume 4, Regency Publications, New Delhi, India, Pg.1931-1934.
39. Simran Kaur , Grover IS, Majar Singh , Antimutagenicity of hydrolyzable tannins from Terminalia chebula in Salmonella typhimurium, Mutation Research, 419, 1998, 169–179.
40. Chia-Lin Chang, Che-San Lin, Development of antioxidant activity and pattern recognition of Terminalia chebula retzius extracts and its fermented products, 2010.
41. Kumar S, Kumar D, Jusha M, Saroha K, Singh N, Vashishta B. Antioxidant and free radical scavenging potential of Citrullus colocynthis (L.) Schrad methanolic fruit extract. Acta Pharmaceutica. 2008;58(2):215-20
42. Zamani M, Rahimi AO, Rezazadeh H, et al. Assessment of anti-hyperlipidemic effect of Citrullus colocynthis. Revista Brasileira de Farmacognosia. 2007;17(4):492-6.
43. Chaturvedi M, Mali PC, . Induction of reversible antifertility with a crude ethanol extract of Citrullus colocynthis Schrad fruit in male rats. Pharmacology. 2003;68(1):38-48
44. Gurudeeban S, Ramanathan T, Satyavani K. Antioxidant and radical scavenging activity of Citrullus colocynthis. Inventi Rapid: Nutracuticlas. 2010;1:38.
45. Jayaraman R, Shivakumar A, Anitha T, Joshi VD, Palei NN. Antidiabetic effect of petroleum ether extract of Citrullus colocynthis fruits against streptozotocin- induced hyperglycemic rats. Rom J Biol Plant Biol. 2009;4:127-34.
46. Kirtikar, K. R and Basu, B. D (1935). Indian medicinal plants. Bishen Singh Mahendra Pal Sigh, Dehradun 1935, vol. III, pp. 1661-1662.
47. Mulliken Ta (2000) implementing CITES for Himalayan medicinal plants ardostachys grandiflora and picrorhiza kurroa in TRAFFIC Bulletine 18,63-72
48. Zhang YJ, Li W & Zheng M (1994). Chinese-English Chinese Traditional Medicine World Dictionary. Shanxi People’s Press, Shanxi, China.
49. RatheeD, Phytochemical screening & antimicrobial activity of Picrorrhiza kurroa an Indian traditional plant used to treat chronic Diarrhoea. http://dx.doi.org/10.1016.arjc.2012.02.009
50. Kumar PV ,(2010) Invitro Antibactrial Activites of Picrorhiza kurroa Rhizome Extract using well Diffusion method . int J pharm Res 2 (1): 30-30
51. Kumar MH, Antimutagenic activity of root extract of Picrorhiza kurroa using Ames test in both Dose Dependant Cytotoxic Assay & Mutagenicity study pharmacogn phytichem 2(6): 48-52
52. Yamgar S,. Studies on Nephroprotective and Nephrocurative Activity of Ethanolic Extract of Picrorhiza kurroa Royle and Arogyawardhini Bati in Rats. Int J Pharm Technol 2(3): 472-489.
53. Pandey BL(1989). Immunopharmacological Studies on Picrorhiza kurroa Royle ex Benth. Part IV: Cellular Mechanisms of Anti-Inflammatory Action. Indian J Physiol Pharmacol 33(1): 28-30.
54. Sinha S, Bhat J, (2011). Hepatoprotective Activity of Picrorhiza kurroa Royle ex Benth. Extract Against Alcohol Cytotoxicity in Mouse Liver Slice Culture. Int J Green Pharm 5: 244-253.
55. Sidhu, G.S., Singh, A.K., Thaloor, D, Banaudha, K.K., Patnaik, G.K. & Srimal, R.C. (1998). Enhancement of wound healing by curcumin in animals. Wound Repair Regen. 6:167-177
56. Hussain, M.S. & Chandrasekhara, N. (1994). Biliary proteins from hepatic bile of rats fed curcumin or capsaicin inhibit cholesterol crystal nucleation in supersaturated model bile. Ind. J. Biochem. Biophy. 31(5): 407-412
57. Deodhar, S.D., Sethi, R. & Srimal, R.C. (1980). Preliminary study on antirheumatic activity of curcumin (diferuloyl methane). Indian J. Med. Res. 71: 632-634.
58. Gukovsky, I., Reyes, C.N., Vaquero, E.C.. (2003). Curcumin ameliorates ethanol and nonethanol experimental pancreatitis. Am. J. Physiol. Gastrointest. Liver Physiol. 284: 85-95.
59. Egan, M.E., Pearson, M., Weiner, Du, K., Lukacs, G.L. & Caplan, M.J. (2004). Curcumin, a major constituent of turmeric, corrects cystic fibrosis defects. Science 304(5670): 600-602
60. Phan, T.T., Sun, L., Bay, B.H., Chan, S.Y. & Lee, S.T. (2003). Dietary compounds inhibit proliferation and contraction of keloid and hypertrophic scar-derived fibroblasts in vitro: therapeutic implication for excessive scarring. J. Trauma 54(6): 1212-1224.
61. Sharma P, Samhita C. Chaukhambha Orientalia. Varanasi: 1992. p. 2. Su.4.3, 12.14, Ci. 6.26, 28. [Google Scholar]
62. Fronties in pharmacology Maria. A. Neag 21 august 2018 volume 91 Articles 557 Neag.etal doi10.3389/fphar.2018.00557 www.frontiersin.org
63. Vaagbhata, Ashtanghridayaam, Commentary by Arunadatta & Hemaadri, collected by Kunt & Narvare and Edited by Paradkara, (Chaukhambha Orientalia, Varanasi & Delhi), 1982.
64. Sushruta, Sushruta Samhita, commentary by Dalhana, Edited by Jadavji Trikamji Acharya, (Chaukhambha Orientalia, Varanasi & Delhi), 1992.
65. Charka, Charaka Samhita, Part I & II, (Hindi commentary by Pandey & Chaturvedi), Edited by Rajeshwar Datta Shastri, (Chaukhambha Vidyabhawan, Varanasi), 1961.
66. Misr.a B. Bhava Prakash Nighantu, Vol. 1, (Hindi commentary by K C Chunekar), (Chowkhamba Vidya Bhavan, Varanasi), 1969: 269.
67. Aiyer K N; Kolammal M. Pharmacognosy of Ayurvedic Drugs of Kerala, (Central Research Institute Trivendrum) 1963; 1:28
68. The Wealth of India, Raw Materials; Publication & Information Directorate, Council of Scientific & Industrial Research: New Delhi 1982; 10: 252
69. B. Halliwell and J. M. Gutteridge, “Lipid peroxidation: a radical chain reaction,” Free Radical Biology & Medicine, vol. 2, pp. 188–218, 1989
70. Z. H. Israili, “Antimicrobial properties of honey,” American Journal of Therapeutics, vol. 21, no. 4, pp. 304–323, 2014.
71. R. J. Whitley, D. W. Kimberlin, and B. Roizman, “Herpes simplex viruses,” Clinical Infectious Diseases, vol. 26, no. 3, pp. 541–553, 1998.
72. L. Vandamme, A. Heyneman, H. Hoeksema, J. Verbelen, and S. Monstrey, “Honey in modern wound care: a systematic review,” Burns, vol. 39, no. 8, pp. 1514–1525, 2013.
73. P.V. Sharma, Dravyagun vigyan, vol- 2, page. 697, Chaukhambha Visvabharati,Reprint 2013
74. P.V. Sharma, Dravyagun vigyan, vol- 2, page. 331, Chaukhambha Visvabharati,Reprint 2013
75. P.V. Sharma, Dravyagun vigyan, vol- 2, page. 753, Chaukhambha Visvabharati,Reprint 2013
76. P.V. Sharma, Dravyagun vigyan, vol- 2, page. 758, Chaukhambha Visvabharati,Reprint 2013
77. P.V. Sharma, Dravyagun vigyan, vol- 2, page. 239, Chaukhambha Visvabharati,Reprint 2013
78. P.V.Sharma, Dravyagun vigyan, vol- 2, page.436 , Chaukhambha Visvabharati, Reprint -2013.
79. P.V.Sharma, Dravyagun vigyan, vol- 2,page. 69 , Chaukhambha Visvabharati, Reprint -2013.
80. P.V.Sharma, Dravyagun vigyan, vol- 2,page.443 , Chaukhambha Visvabharati, Reprint -2013.
81. P.V.Sharma, Dravyagun vigyan, vol- 2,page.162 , Chaukhambha Visvabharati, Reprint -2013.
82. P.V. Sharma, Dravyagun vigyan, vol- 2, page. 537, Chaukhambha Visvabharati,Reprint 2013
83. P.V.Sharma, Dravyagun vigyan, vol-2, page.761, Chaukhambha Visvabharati,Reprint 2013
84.P.V. Sharma, Dravyagun vigyan, vol-2,page. 202, Chaukhambha Visvabharati,Reprint 2013
85. Kirtikar KR, Basu BD, editors. Indian Medicinal Plants, Vol 1. 2nd ed. New Connaught Place, Dehra Dun: M/S Bishen Singh, Mahendra Pal Singh; 1975
86. Nayampalli S, Ainapure SS, Nadkarni PM. Study of antiallergic acid Bronchodilator effects of Tinospora cordifolia. Indian J Pharm 1982; 14:64-6.
87. Janey Alam Journal of Applied Pharmaceutical science Volume 5(08) Pp173-181 Aug 2015, Doi:10.73241/JAPS.2015.50827 , ISSN2231-3354, http://www.japsonline.com
88. Prusti AB and Behera KK: Ethnobotanical Exploration of Malkangiri District of Orissa, India. Ethnobotanical Leaflets, 2007; 1:12-15.
89. Yesodharan K : Ethnomedicinal knowledge among Malamalasar tribe of Parambikulam wildlife sanctuary, Kerala. Indian J. of Traditional Knowledge, 2007; 6(3): 481-485.
90. Kore KJ, Shete RV , Desai NV: Anti-arthritic activity of hydroalcoholic extract of Lawsonia inermis, International Journal of Drug Development and Research, 2011; (3): 217-224.
91. Hussain A.R. Henna Ability in Treating Diseases in Prophetic Medicine. 2010. http://www.protectedpearls.com/apps/blog/show/4090948-henna-ability-in-treating-diseases.
92. Munshi S. R., Shetye T. A. and Nair R. K. Antifertility activity of three indigenous plant preparations. Planta Medica.1977, 31(1):73-75.
93. Sathya A, Siddhuraju P. Protective effect of bark and empty pod extracts from Acacia auriculiformis against paracetamol intoxicated liver injury and alloxan induced type {II} diabetes. Food Chem Toxicol. 2013. doi:10.1016/j.fct.2013.02.031
94. Sánchez E, Heredia N, del Camacho-Corona MR, García S. Isolation, characterization and mode of antimicrobial action against Vibrio cholerae of methyl gallate isolated from Acacia farnesiana. J Appl Microbiol. 2013. doi:10.1111/jam.12328.
95. P.V.Sharma, Dravyagun vigyan, vol-2,page.159 , Chaukhambha Visvabharati, Reprint -2013.
96. P.V.Sharma, Dravyagun vigyan, vol-2,page.726 , Chaukhambha Visvabharati, Reprint -2013.
97. P.V.Sharma, Dravyagun vigyan, vol-2,page.195 , Chaukhambha Visvabharati, Reprint -2013.
98. P.V.Sharma, Dravyagun vigyan, vol-2,page.180 , Chaukhambha Visvabharati, Reprint -2013.
99. P.V.Sharma, Dravyagun vigyan, vol-2,page.160 , Chaukhambha Visvabharati, Reprint -2013.
100. Priya VratSharma, Susruta Samhita, volume-2,Chikitsa sthana,chapter 40,verse no- 64,Chaukhambha Visvabharati, Varanasi.
"

